Diabetic Eye Surgery
Living with diabetes can be challenging, and managing the potential eye complications can add another layer of complexity. That’s why we’re dedicated to providing compassionate and comprehensive care for people with diabetes who may be at risk for diabetic eye diseases.
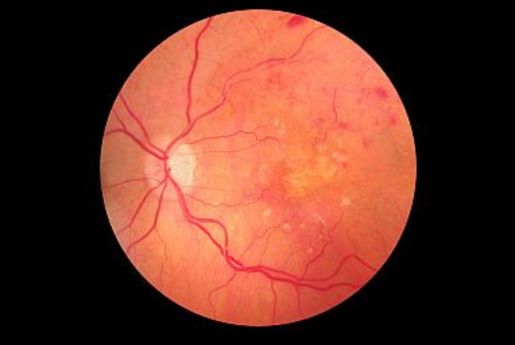
Diabetes affects the neurosensory layer of the eye called the retina. Diabetic retinopathy is prevalent in those who have uncontrolled blood sugar and a long duration of diabetes. Other than this, people with high blood pressure, high cholesterol, kidney disease, heart disease, and a low hemoglobin count are also at risk of developing diabetic retinopathy-related vision loss.
Our ophthalmologists, optometrists, and support staff are committed to helping you manage your diabetes and maintain good eye health. We offer a range of diabetic retinopathy treatments including intravitreal Anti-VEGF injections, laser treatment for diabetic retinopathy, diabetic eye surgery in the form of microincision vitrectomy surgery (MIVS)
Diabetic Retinopathy Treatment: Understanding Your Options
Diabetic retinopathy is a severe condition that affects the blood vessels in the retina and can lead to vision loss if left untreated.
Stages of diabetic retinopathy include –
Non-Proliferative Diabetic Retinopathy – In this early stage of diabetic eye disease, patients usually may not have any symptoms of eye disease. Catching the disease at this stage is of great advantage to the patient and the doctor because, with correct treatment and follow-ups, vision loss can be prevented.
In the nonproliferative stage, some patients may experience dimness of vision due to diabetic macular edema, a swelling in the central part of the retina. This is treatable of intravitreal eye injections or by green laser treatment of the retina (laser photocoagulation).
In Early Proliferative Diabetic Retinopathy (PDR), also called vision-threatening diabetic retinopathy, urgent treatment is required in the form of pan-retinal photocoagulation (A type of laser treatment of the retina). Sometimes intravitreal eye injections or a combination of both laser and injections help restore vision loss.
In Advanced Proliferative Diabetic Retinopathy (PDR), usually retina surgery in the form of vitrectomy (microincision vitrectomy surgery – MIVS) is needed to help restore vision.
Laser Treatment for Diabetic Retinopathy: What You Need to Know
Laser treatment for diabetic retinopathy is a highly effective way to manage the condition and prevent further vision loss. At EyeSite Eye Hospital & Retina Centre, we offer both focal and pan-retinal photocoagulation, two types of laser treatment for diabetic retinopathy.
During focal photocoagulation, the laser treats specific areas of the retina where abnormal blood vessels have formed. Panretinal photocoagulation, on the other hand, treats the entire retina to reduce the number of abnormal blood vessels and prevent further damage.
While laser treatment for diabetic retinopathy is generally safe and effective, there are certain risks and potential side effects in a minority of cases. Our team of experienced ophthalmologists will discuss these with you in detail and help you decide whether laser treatment is appropriate for you.
Intravitreal Eye Injections: What you need to know
Intravitreal Anti-VEGF injections are commonly used safe and effective treatment options for diabetic macular edema and early stages of proliferative diabetic retinopathy. Injection options include Avastin, Accentrix, Razumab, Ozurdex, Pagenax, and Eylea. Sometimes, these injections are repeated at monthly intervals initially and then tapered off to give you the best visual outcome. Your retina doctor will discuss all options with you and help you choose the best for your eyes.
Diabetes and Cataract Surgery: What You Should Know
People with diabetes are at an increased risk of developing cataracts, a clouding of the eye’s natural lens that can cause blurred vision.
Before cataract surgery managing your blood sugar levels before cataract surgery is essential to minimize the risk of complications. Our team will work with you to develop a personalized plan to help you prepare for surgery and will closely monitor your blood sugar levels throughout the process.
Our surgeons will remove the cloudy lens during cataract surgery and replace it with an artificial lens. While cataract surgery is generally safe and effective, people with diabetes may be at an increased risk of complications such as infection and delayed healing. Our team will closely monitor your recovery and provide the necessary support to ensure a successful outcome. We offer specialized diabetic eye surgery to effectively manage vision complications. Our comprehensive services include advanced treatments for diabetic retinopathy, as well as specialized treatments like glaucoma treatment and cornea treatment. Trust our experienced team of ophthalmologists to provide personalized solutions and ensure optimal outcomes for your eye health.
Book an Appointment





Our Specialist Doctor
Meet Dr. Ashutosh Agarwal our in-house vitreoretinal surgeon. Trained at the prestigious Sankara Nethralaya, Chennai, Dr. Ashutosh Agarwal treats his diabetic retinopathy patients with compassion and utmost personal care.
We have the best medical and surgical retina technology in the form of OcuLight green laser (BioMedix USA), Constellation Vision System (Alcon, USA), along with all sorts of intravitreal injections

Why Do People Love Us?
About Eye Site
Freqently Ask Question
Diabetic retinopathy is a complication of diabetes that affects the blood vessels in the retina, the light-sensitive tissue at the back of the eye. Over time, high blood sugar levels can damage the blood vessels, leading to vision problems and, in severe cases, blindness.
In its early stages, diabetic retinopathy may not cause any symptoms. However, as the disease progresses, symptoms may include blurred or distorted vision, floaters (dark spots or strings that appear to “float” in the field of vision), and difficulty seeing in dim light or at night.
Diabetic retinopathy is typically diagnosed during a comprehensive eye exam. Your eye doctor will examine the retina and may perform tests such as a dilated eye exam, retinal photography, or optical coherence tomography (OCT) to assess the blood vessels and structures in the eye.
The best treatment for diabetic retinopathy depends on the severity of the disease. In its early stages, managing blood sugar levels and blood pressure can help to slow the progression of the disease. If vision loss has occurred, laser surgery may be recommended to seal leaking blood vessels or to shrink abnormal blood vessels. In some cases, injections of medications called anti-VEGF agents may be used to reduce swelling and inflammation in the eye. It’s important to work closely with your eye doctor to develop a treatment plan that is appropriate for your individual case.
What we do
We Provide Awesome Services
Get rid of your glasses quicly and effectively.
Contact us to know more
At Eye Site Eye Hospital, we are dedicated to providing comprehensive eye care services with cutting-edge technology and a compassionate approach. Whether you’re seeking routine eye care or specialized treatment, our team of experienced ophthalmologists is committed to offering the highest standards of care for all patients.
Diabetic Retina Specialist in Indore
Diabetic retinopathy is a serious eye condition affecting individuals with diabetes, potentially leading to vision loss if left untreated. At Eye Site Eye Hospital, we have a dedicated diabetic retina specialist in Indore who is highly skilled in diagnosing and treating all stages of diabetic retinopathy. Our specialist uses advanced diagnostic tools such as retinal imaging to detect early signs of retinopathy and create personalized treatment plans to preserve your vision.
If you are living with diabetes, regular eye check-ups are crucial to maintaining your eye health. Our diabetic retina specialist works closely with patients to manage their condition and provide effective treatments, including laser therapy, injections, and surgery.
Best Eye Hospital for Diabetic Retinopathy
Eye Site Eye Hospital is widely recognized as the best eye hospital for diabetic retinopathy in Indore. We combine state-of-the-art facilities with expert care to deliver the best outcomes for our patients. Our hospital is equipped with the latest technologies for the treatment of diabetic retinopathy, allowing us to offer a range of advanced treatments in a comfortable and safe environment.
Our commitment to excellence has earned us the trust of countless patients who have received life-changing treatments at our hospital. Whether you require laser treatment, anti-VEGF injections, or vitrectomy surgery, our experienced team is here to guide you through every step of your eye care journey.










